Knee Pain - Changing Focus
Knee Pain: What Are We Actually Treating?
Knee pain is one of the most confidently diagnosed problems in musculoskeletal practice. We’ve all seen what will for many be a familiar list: meniscal tears, medial collateral ligament strains, patello-femoral pain, osteoarthritis, pes anserinus bursitis.
All of these will undergo imaging to create the label and the treatment will follow accordingly, whether it be manual intervention, Instrument Assisted Massage-IAMs, taping, injection, surgery, exercise and so forth.
This structural model has obvious strengths and advantages. Acute trauma needs identifying swiftly and flags that raise other issues matter greatly. Surgical repair in the form of ACL or total replacements have dramatically transformed lives. None of this is in dispute.
But once we step outside the acute injury or the obvious need for replacement, something interesting happens.
Knees can hurt without any clear structural correlation or a surgical imperative.We see MRI findings in people with no symptoms or with identical findings from images, who function very differently from each other.(Englundet al., 2008)
We also see pain persisting long after tissue healing timelines have passed. At this point, the purely local model begins to crack.
This doesn’t mean the structures suddenly stop mattering however. Cartilage, ligaments, bone surfaces and the meniscus all remain very real tissues with very real loading limits and damage to any of them is going to hurt. Sometimes the appropriate answer really is surgical repair.
But once we accept that similar structures can produce very different experiences of pain, the obvious question becomes this: what else is influencing the system?
The knee is often described as a 'modified hinge joint' with supporting ligaments and cartilage surfaces. Although anatomically, this is correct in a narrow sense, it’s functionally pretty incomplete.
Rather than viewing the knee as an isolated hinge, we need to consider it more as being a load transfer station between foot and hip, influenced by trunk control, habit, confidence, fatigue, and of course my favourite word, context.(Powers, 2010)
As I’ve discussed before, pain is not simply a tissue report but is an output.(Explain Pain Second Edition - NOI Group,)It represents the nervous system’s interpretation of what is happening within the body and whether that situation represents a threat to the organism.
In other words, nociception may provide information about tissue stress or irritation, but the experience of pain is the nervous system’s response to that information, combined with context.
That context is wide. It includes previous injury, expectations about what pain means, confidence in movement, sleep quality, fatigue, stress, cultural beliefs about damage, and the simple question of whether someone feels safe to move.(Wiech 2016,Deconstructing the sensation of pain: The influence of cognitive processes on pain perception)
If that sounds abstract, consider what might be a familiar presentation to many of you: two people present with similar medial knee pain and similar degenerative findings on imaging. One continues to hike and garden. The other avoids stairs and believes their knee is “worn out.” The tissue findings may be comparable, but their lived experience is wildly different. In either case the knee itself hasn’t changed very much, but the conditions surrounding its use have.
Once behaviour and protection strategies enter the picture, the knee is no longer just a hinge with a problem, but becomes part of a wider system negotiating load and safety.
For me, this is where the conversation becomes more interesting.
When we dissect knees we tend to isolate structures for clarity: quadriceps tendon, patella, menisci, collateral ligaments, pes anserinus and so forth.
In reality, these structures, like most tissues in the body, don’t operate as neatly separated units. Tendons blend into fascia, fascia blends into retinacula, and forces spread across tissues in directions that are far more complex than the compartmentalised diagrams anatomy could ever show.
Imaging introduces another simplification. An MRI or X-ray captures a static image of a structure that is unloaded and not moving. The person lies still while the scan is taken and what we see afterwards is a snapshot of tissue shape at that moment in time.(Brinjikjiet al., 2015)
Sometimes of course these images reveal clear structural damage, and when they do they can be extremely useful. But whether an image shows something obvious or nothing remarkable at all, it still tells us very little about the lived experience of the person whose knee we are looking at.
Images cannot show how someone moves, how they protect the joint, or how the knee behaves when it is actually under load. They don’t show the subtle adjustments people make when they walk, climb stairs, kneel, or simply try to get through a day with less discomfort. Nor can they tell us what the pain means to that person, or how it has altered their confidence in using the joint. How they struggle to care for a loved one or worry about losing work hours.
In other words, imaging can show us structure, but it can’t tell us the human story of the knee that structure belongs to. It also tends to keep our attention fixed on local structures rather than encouraging us to think about how load is being managed across the wider system.
A good example is the group of muscles known as pes anserinus.
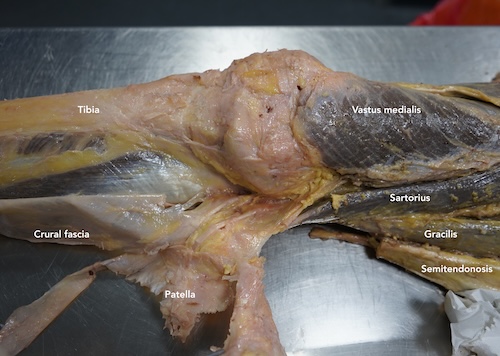
This area is usually described simply as the insertion of three tendons,sartorius, gracilis and semitendinosus,onto the medial tibia, occasionally accompanied by the mention of a small bursa that may become irritated. In textbooks it often appears as a relatively minor anatomical detail.
When you look at real tissue rather than diagrams however, something else becomes obvious. Rather than sitting in isolation the pes anserinus blends into fascial layers that form a continuity toward and over the anterior knee and the patella.
This observation alone doesn’t magically explain all knee pain or indeed provide any solutions. It does, however, remind us that what we think of as ‘the knee’ is part of a continuous load-sharing system rather than a collection of disconnected parts.
Focusing exclusively on the local structure or the location of pain, may therefore sometimes miss the larger pattern of how load is being negotiated.
Once behaviour, perception and structural continuity are added into the picture, the original question — “what is damaged in the knee?” — becomes only one of any number of useful questions.
We might also ask what events preceded the current presentation. Was there a gradual lead-up to the pain, or did it appear suddenly? What were the conditions surrounding the incident? Have there been previous injuries, changes in activity, or shifts in confidence that might have altered how the knee is being used?
A recent example illustrates the point. When Lindsey Vonn crashed at the Milan Winter Olympics, many ‘expert biomechanists’ immediately began analysing the seconds leading up to the incident, looking for subtle loading errors that might explain what had happened. She had already ruptured her left ACL the previous week, and it was assumed by many that this injury must have been responsible for the fall.

It may well have contributed as previous injury almost always influences how someone loads and moves. But in this case the immediate cause was rather more straightforward: she caught her arm in a slalom gate at high speed.
For someone like me, however, the more interesting question begins after the crash. What influence will her previous injury, her history and her own perception of the event have on how she loads and trusts that knee in the future?
Everything from falling off a bike at twelve to straining a shoulder in the gym last year becomes part of that story. Each experience contributes to how someone moves, what they trust their body to do, and how confidently they place load through the joint. My focus then becomes not whether this is a meniscus or MCL issue, but rather, “what is this person’s knee responding to, and what would allow a more confident and less protective function?”
This shift in perspective doesn’t abandon structural diagnosis, because at the end of the day structure still matters. But structure rarely, if ever tells the whole story. My suggestion instead is that we recognise a simple fact: ‘knees’ exist inside people, and people don’t function as isolated hinges.
References
Brinjikji, W.et al.(2015) ‘Systematic Literature Review of Imaging Features of Spinal Degeneration in Asymptomatic Populations’,American Journal of Neuroradiology, 36(4), pp. 811–816. Available at: https://doi.org/10.3174/ajnr.A4173.
Deconstructing the sensation of pain: The influence of cognitive processes on pain perception(no date). Available at: https://doi.org/10.1126/science.aaf8934.
Englund, M.et al.(2008) ‘Incidental Meniscal Findings on Knee MRI in Middle-Aged and Elderly Persons’,New England Journal of Medicine, 359(11), pp. 1108–1115. Available at: https://doi.org/10.1056/NEJMoa0800777.
Explain Pain Second Edition - NOI Group(no date). Available at: https://www.noigroup.com/product/explain-pain-second-edition/ (Accessed: 24 March 2021).
Powers, C.M. (2010) ‘The Influence of Abnormal Hip Mechanics on Knee Injury: A Biomechanical Perspective’,Journal of Orthopaedic & Sports Physical Therapy, 40(2), pp. 42–51. Available at: https://doi.org/10.2519/jospt.2010.3337.

