Rethinking Shoulder Pain
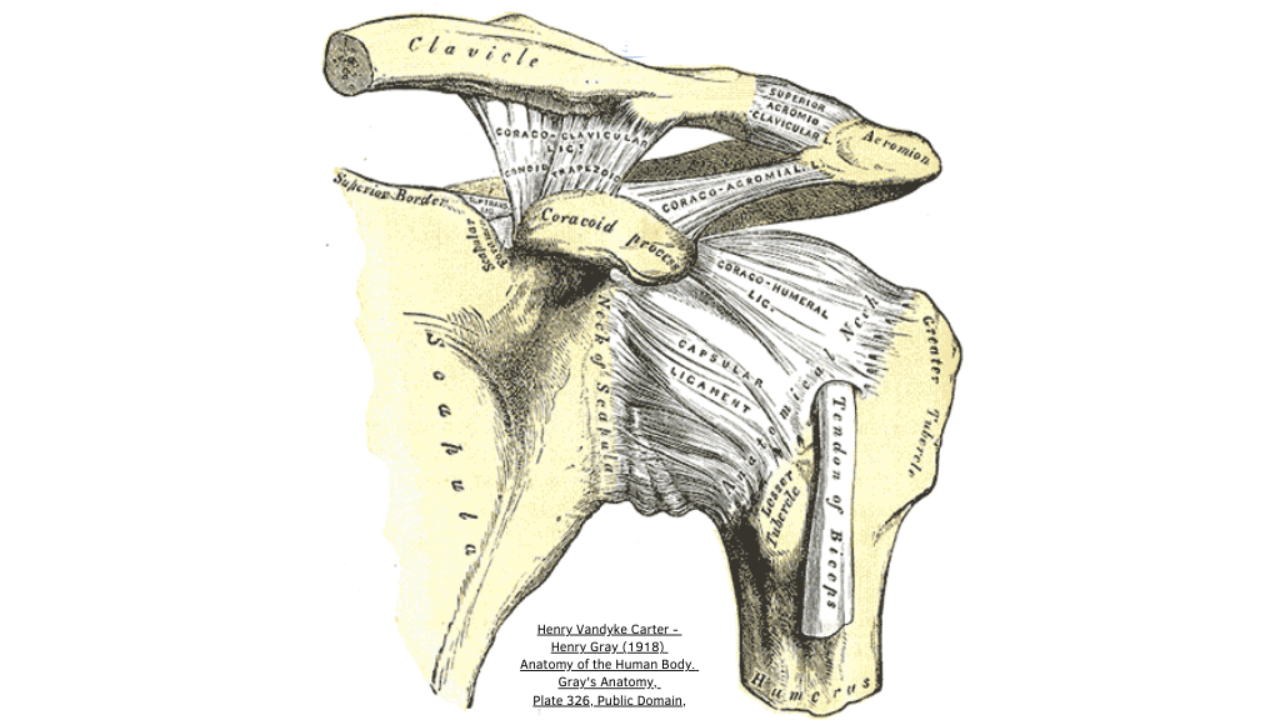
The Shoulder - Not just a ball and socket joint
Spend enough time around people in pain and patterns tend to emerge. Not structural patterns in the way that we’re told exist (and which may or may not), but behavioural ones.
These are natural enough to understand and spot when treating. Guarding, holding on when we’re trying to move passively with someone. A sense of needing to control the tissue of interest.
A recent case I was working with is a good example. It was someone with acute shoulder pain, but also a shoulder that wouldn’t move passively. This wasn’t because it couldn’t move, but because for some reason it just wouldn’t let go. The muscle activity just sat there like a constant background hum, being protective of the area and yet also completely outside her conscious awareness.
From experience I know that trying to tell someone to “relax” is just going to be annoying and pointless for us both, but also realise that this pattern of holding for people in pain, is both common and exhausting. The tissues involved are expending enormous amounts of energy and the stress, fear and tension around what will inevitably be sharp pain at some point, soon drains the client.
An approach that helped, was as with many things, alarmingly simple and called on some visualisation. I asked her to put one knee on a chair and then let her arm hang loose. Not heavy or with a weight, but as if her arm was a rag or piece of rope hanging from a branch.
From here we just then let it wobble and wave, as if being blown like a willow in the breeze. What appeared in a short time was something that she hadn’t experienced for quite some time: an absence of effort.
The months of subconsciously guarding her arm and shoulder as an erroneous form of protection was, at least for a brief window, no longer present. It wasn’t so much the absence of pain in that moment that was striking, but the comment that it felt like a “weight had been taken away, as if being relieved of a heavy bag of shopping.”
For me, this is the point that reframes the idea of what a shoulder is, away from the mechanical principles of the joint and ligaments that make it up.
The over-simplification problem
The classic shoulder model is familiar: the glenohumeral joint as a ball and socket, making for a tidy bit of engineering. A clear, movable interface between humerus and scapula.
It’s a useful model but barely close to being sufficient in terms of understanding movement, implying as it does that movement happens at the joint. In reality, even the smallest of shoulder movements are whole body events dependent on a complex series of interactions (Hodges & Tucker, 2011; Latash, 2012) including;
Scapular positioning and timing
Thoracic rotation and extension
Rib movement and breathing mechanics
Cervical spine contribution
And crucially, the nervous system deciding what movement is safe
Focus only on the glenohumeral joint and we’re observing a solo violin in a system that behaves more like an orchestra.
A busy system not a stiff one
In my client, her limitation isn’t mechanical in the traditional sense, but could be more accurately described as an “overactivity response.” Because her shoulder musculature was already “on”, it meant that passive movement wasn’t really passive.
Any manual or movement therapy approach is an interaction with an active system, and any intervention is layered on top of whatever contraction might be present. So what we refer to as “restriction” might better be understood as ongoing motor output (Hodges & Tucker, 2011).
We hear the phrase repeated that something feels “tight”, but a better thought might be “why is this part of the system choosing to be overactive?”
Think action potentials before adhesion
At the cellular level, muscle contraction is driven by electrical signalling, action potentials triggering calcium release and cross-bridge cycling (Hall & Guyton, 2021). So far so uncontroversial.
What’s often missed, however, is that as well as this process being able to produce and effect movement, it can also logically prevent it. The nervous system is perfectly capable of maintaining low-level, sustained contraction as a protective strategy. In pain states, this can become persistent, even when the original pain trigger has long gone (Hodges & Tucker, 2011).
Research into pain science makes it clear that pain is not a direct readout of tissue damage, but rather an output of the brain, informed by context, expectation and perceived threat (Butler & Moseley, 2013).
If a system interprets movement as risky, it doesn’t wait for damage to occur. It preloads tension into the area as a preventative measure.
What the ‘raggedy arm’ method achieved
Letting the arm hang loosely did something deceptively simple, that of removing the requirement of the system for control. There was no outcome to the task involved and no expectation or requirement of precision present. In this loose, hanging position gravity was replacing the need for muscular tension to be present.
From here, motor output to the area would begin to down-regulate, the system would receive a different sensory input and the perceived need for protection would reduce.
When she stood back up, there was no change to the actual tissue. However, in that brief window of time, there was an absence of what was there normally, contraction, giving the system a glimpse of what might be needed to allow change to occur.
Like knees, most shoulders have some degree of structural change, even if no pain is being reported. It might be that repeating this process regularly would be enough to reduce symptoms, or at least allow for more effective treatment.
The ever-present neck
Another reason to look beyond the glenohumeral space is that shoulder presentations rarely appear in isolation from neck restrictions, neck pain or pointers towards a historical issue in the cervical spine.
Anatomically speaking, this is hardly a coincidence. The cervical spine and shoulder share neural supply via the brachial plexus, as well as a significant degree of muscular overlap such as the trapezius and levator scapulae (Sterling, 2011).
Restricted lateral flexion in the neck isn’t therefore a localised issue, but reflects these relationships and the way that the shared system organises movement and protection across multiple regions.
The thoracic spine gets a mention
Moving further down, limited rotation in the thoracic region changes how the shoulder has to behave.
If the thorax isn’t moving, the scapula has fewer options, meaning that the humerus is required to compensate in ranges where it might not otherwise be asked to. The likely result is an increase in muscle tone as the system attempts to stabilise this altered demand.
Breathing adds another non-optional dimension. The ribs, diaphragm and thoracic spine are mechanically and neurologically linked. Alter breathing patterns through pain or other factors and you alter thoracic movement, which in turn influences shoulder behaviour.
We aren’t discussing separate systems here, but different views of the same one.
Context is my favourite word
What this approach to shoulder pain highlights is something still underrepresented in many areas of clinical thinking. Pain doesn’t exist in joints, muscles or any structure for that matter, but is a product of systems.
A constantly “switched on” shoulder isn’t just a musculoskeletal issue, but could be better understood as a neuro-behavioural state (Green et al., 2023).
This change in thinking influences everything.
How movement feels
How manual therapy is received
How quickly change occurs
Working into a system that’s already guarding is like trying to stretch a muscle that’s actively contracting. You’re not starting from neutral, and any intervention is more likely to be resisted.
In conclusion
Calling the shoulder a ball and socket joint isn’t wrong, it’s just incomplete. When taken in isolation as the subject of treatment, surgery or rehabilitation, it misses the wider context of how systems interact and how behaviour and perception influence outcomes.
Sometimes the most meaningful approach isn’t adding something to what may already be an overloaded system, but taking something away in terms of effort or control.
Reducing unnecessary activity rather than forcing range might be a more useful place to start.
References
Butler, D. S., & Moseley, G. L. (2013). Explain Pain. NOI Group.
Green, J., et al. (2023). Neurobehavioural mechanisms of pain and movement. Frontiers in Pain Research. [https://pmc.ncbi.nlm.nih.gov/articles/PMC10330476/](https://pmc.ncbi.nlm.nih.gov/articles/PMC10330476/)
Hall, J. E., & Guyton, A. C. (2021). Guyton and Hall Textbook of Medical Physiology. Elsevier.
Hodges, P. W., & Tucker, K. (2011). Moving differently in pain: a new theory to explain the adaptation to pain. Pain, 152(3), S90–S98.
Latash, M. L. (2012). The bliss (not the problem) of motor abundance. Experimental Brain Research, 217(1), 1–5.
McGill, S. (2016). Low Back Disorders. Human Kinetics.
Sterling, M. (2011). Physiotherapy management of whiplash-associated disorders. Journal of Physiotherapy, 57(1), 5–12.

